In this Medical Monday series, we’re talking about how your doctor reaches a diagnosis of common conditions associated with coagulation. It may help if you first read the introduction, before reading about today’s topic of thrombophilia. Altogether we’re covering
- Introduction
- DVT, Deep Vein Thrombosis
- Post-thrombotic syndrome
- PE, Pulmonary Embolism
- Pulmonary hypertension
- AF, Atrial Fibrillation
- Heart Valve conditions – aortic and mitral
- Thrombophilia
- Stroke
Introduction
Thrombophilia is really a misnomer as it means “a love of thrombosis or blood clots”, however it is used to describe people with an increased risk of thrombosis. Some conditions are inherited so are present from birth and can run in families, whereas others are acquired and often the cause is unknown.
It has been known for a long time that there are some families with a high risk of blood clots but it is only in the last 30-40 years that doctors have started to unravel the causes. We still only find the cause in about 50% of people. The conditions that are associated with an increased risk of clots are deficiencies of certain clotting proteins – antithrombin deficiency, protein C deficiency and protein S deficiency – and mutations in factor V (factor V Leiden) and the prothrombin gene. Although we know a lot about these conditions, it is questionable if there is any value in testing for them. If you have had one blood clot and have an inherited disorder, your risk of another clot is no different from somebody without one of these conditions, and if you have had more than one blood clot you probably need to remain on long-term treatment whether you have a thrombophilia or not. So making the diagnosis doesn’t make any difference to your treatment. As a results many doctors do not test for these conditions as the tests are expensive and the results don’t alter treatment.
The other major thrombophilia is lupus anticoagulant which can be part of the antiphospholipid syndrome. This is an acquired condition and is associated with a high risk of blood clots. It is worth knowing about this condition as long-term treatment is recommended even after one blood clot.
Your story
 Your story will be the same as somebody with a deep vein thrombosis or a pulmonary embolus but you may have a family history of blood clots. It is interesting that a lot of people do not know if they have a family history and only find out after they have had a clot. If you have had a clot, it is worth asking around your family to see if other family members are affected; it can be important for your family. If you have an inherited disorder and have daughters, you should advise them to avoid the oral contraceptive as this can increase their risk of clots.
Your story will be the same as somebody with a deep vein thrombosis or a pulmonary embolus but you may have a family history of blood clots. It is interesting that a lot of people do not know if they have a family history and only find out after they have had a clot. If you have had a clot, it is worth asking around your family to see if other family members are affected; it can be important for your family. If you have an inherited disorder and have daughters, you should advise them to avoid the oral contraceptive as this can increase their risk of clots.
Tests you may have
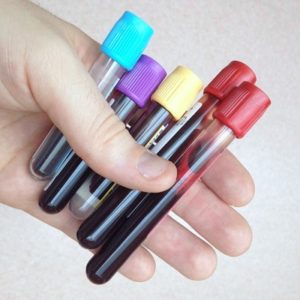 The various forms of thrombophilia are diagnosed with a blood test, however many of these tests cannot be performed when you are taking anticoagulants. You will probably havo wait until you have stopped taking an anticoagulant before the tests can be performed. The genetic tests such as the factor V Leiden and the prothrombin gene test give a definite answer; you either have the mutation or you don’t, but it can be hard to interpret some of the other tests. Often the results are borderline and need to be repeated to confirm the diagnosis.
The various forms of thrombophilia are diagnosed with a blood test, however many of these tests cannot be performed when you are taking anticoagulants. You will probably havo wait until you have stopped taking an anticoagulant before the tests can be performed. The genetic tests such as the factor V Leiden and the prothrombin gene test give a definite answer; you either have the mutation or you don’t, but it can be hard to interpret some of the other tests. Often the results are borderline and need to be repeated to confirm the diagnosis.
The diagnosis of lupus anticoagulant and the antiphospholipid syndrome can be very difficult. Lupus anticoagulant is an acquired antibody that affects the way your blood clots. It can be detected using a number of different of clotting tests, most laboratories perform two different tests. These can be hard to interpret and are often give borderline results. You may need to have tests repeated two or three times before your doctor is sure you have this condition. It is important to get the diagnosis right as people with this condition often need long-term anticoagulants.
Have you had thrombophilia testing?
Did you find testing helpful?


Leave a Reply