Pregnancy
 Deep vein thrombosis and pulmonary embolus are serious complications of pregnancy. They are potentially life-threatening and can lead to long-term complications. Pulmonary embolus is the commonest cause of maternal death in most developed countries, so being aware of the risks and signs is very important.
Deep vein thrombosis and pulmonary embolus are serious complications of pregnancy. They are potentially life-threatening and can lead to long-term complications. Pulmonary embolus is the commonest cause of maternal death in most developed countries, so being aware of the risks and signs is very important.
Increased risk of clotting
Pregnancy is sometimes referred to as a prothrombotic condition. That means that during pregnancy there are changes in the blood that increase the risk of blood clots. These are complex and involve changes in the clotting factors, changes in fibrinolysis (the ability to break down blood clots) and changes in blood flow. Venous flow from the leg has been measured at a rate three times slower than in the non-pregnant state. These changes are largely driven by hormonal changes. This may be a normal physiological state to stop bleeding after delivery but can potentially be dangerous. The risk of a DVT or PE is about 5 times higher during pregnancy compared to a woman who is not pregnant with an incidence of about 1 in every 2,000 pregnancies.
When do clots occur?
 Blood clots can occur at anytime during pregnancy and occur at a similar frequency in all trimesters, but some series have suggested that the risk is highest during the early stages of pregnancy with about 50% occurring before 15 weeks, whereas others suggest the risk increases progressively during pregnancy. The highest incidence of a blood clot is during the first 3 weeks after delivery. During this period the risk of a blood clot is about 25 times higher than in the non-pregnant state.
Blood clots can occur at anytime during pregnancy and occur at a similar frequency in all trimesters, but some series have suggested that the risk is highest during the early stages of pregnancy with about 50% occurring before 15 weeks, whereas others suggest the risk increases progressively during pregnancy. The highest incidence of a blood clot is during the first 3 weeks after delivery. During this period the risk of a blood clot is about 25 times higher than in the non-pregnant state.
Where do clots occur?
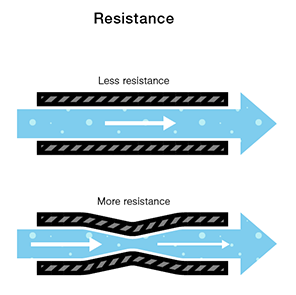 Interestingly approximately 80% of DVTs in pregnancy occur in the left leg. This is due to the anatomy of the blood supply to the legs. The right common iliac artery crosses over the left iliac vein. During pregnancy it is thought that the artery compresses the vein slowing blood flow. Compression is partly due to the enlarged uterus.
Interestingly approximately 80% of DVTs in pregnancy occur in the left leg. This is due to the anatomy of the blood supply to the legs. The right common iliac artery crosses over the left iliac vein. During pregnancy it is thought that the artery compresses the vein slowing blood flow. Compression is partly due to the enlarged uterus.

Leave a Reply