When you’re on anticoagulants, you may have concerns that you’re not quite sure if you should be bothering your doctor with.
My patients often bring up these concerns towards the end of a visit often prefacing them with “Am I being silly doctor?” I feel that although my work as a haematologist can be very busy, answering a patient’s questions is a core part of my job, so I’d rather patients tell me their concerns rather than silently worrying because they don’t want to bother me. Having said that some concerns are more dangerous than others, so today I’m covering the middle of a series of 3 posts over 3 Mondays on concerns that are;
- Life-threatening
- Valid
- Niggling
Today’s concerns are those that are worth mentioning to your doctor but are unlikely to be life-threatening.
1. I took the wrong dose of tablets
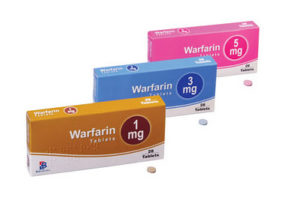 It can be easy to mix up the colours of the warfarin tablets you should be taking, or take your tablets twice as you forgot you’d already taken them. On most occasions mixing up your tablets is not too serious. If you forget to take your tablets but remember later the same day then take them as soon as you remember. If you don’t realise you have missed your tablets until the next day, do not double up your dose, just take your dose for that day.
It can be easy to mix up the colours of the warfarin tablets you should be taking, or take your tablets twice as you forgot you’d already taken them. On most occasions mixing up your tablets is not too serious. If you forget to take your tablets but remember later the same day then take them as soon as you remember. If you don’t realise you have missed your tablets until the next day, do not double up your dose, just take your dose for that day.
If you are sure you have taken the dose twice on the same day don’t worry. Warfarin has a slow effect on the way your blood clots so your risk of bleeding is low. I usually recommend missing the dose the next day just to be safe, but if you are worried talk to your doctor.
If you realise you have been taking the wrong dose for some time you need to talk to your doctor. I have occasionally had patients who have taken 5 mg for several days before they realised they should be taking 1 mg! I would recommend getting an INR test as soon as possible in this case and if the INR is very high you may need vitamin K.
2. I started antibiotics, could that interfere with my warfarin dose?
 Many medications interact with warfarin particularly antibiotics. Your pharmacists will usually tell you if an interaction is likely. The difficult thing with warfarin and antibiotics is that the effect on the INR can be very variable. For example some people can take penicillins and it will have no affect on their INR and for other people the INR will go really high.
Many medications interact with warfarin particularly antibiotics. Your pharmacists will usually tell you if an interaction is likely. The difficult thing with warfarin and antibiotics is that the effect on the INR can be very variable. For example some people can take penicillins and it will have no affect on their INR and for other people the INR will go really high.
A short course of antibiotic for just a few days is unlikely to have much effect, but a longer course can cause problems. I usually recommend getting an INR check 3 to 4 days after starting antibiotics. If the antibiotic is going to affect the INR you will know by then and if there is no change in the INR you are probably safe to continue. A few antibiotics make the INR lower than normal; check with your pharmacist. Also remember if you have a long course of antibiotics and your warfarin dose has been changed while you are taking them, you will need to check the INR again after stopping the antibiotics.
3. What should I do about my medication before having surgery?
If you are taking warfarin or one of the newer anticoagulants you may need to stop your treatment before surgery. For minor procedure like removing small moles or skin lesions you can often continue anticoagulants but you should check with your doctor. For more major surgery you should be given a plan by the hospital. This may involve stopping treatment for a few days before surgery or you may need to change to heparin or low molecular weight heparin injections before surgery. The important thing is that you have a plan and that your doctor is aware you are on an anticoagulant. In hospital it is not uncommon for patients to arrive for surgery still on their warfarin because nobody told them to stop. When this happens the surgery has to be canceled which is upsetting for everybody.
4. What should I do about my medication before going to the dentist?
You normally do not need to do anything about your anticoagulants if you are going for a routine check-up or a scale and polish, but if you are having anything more major done you should tell your dentist you are on an anticoagulant.
Even if you are going to have an extraction you may not need to stop your treatment, most dentists are happy to do a simple extraction if you are on anticoagulants. However for anything more major your dentist will want you to stop treatment for one or two days. If you have recently had a blood clot, heart attack or heart surgery you should make sure your dentist contacts your doctor to check that it is OK to stop your anticoagulant.
5. I’ve had food poisoning, will that affect my medication?
Food poisoning can put you off your food, make you vomit and cause diarrhoea; all of these can affect your INR (if you are on warfarin). A short bout of food poisoning is unlikely to have much impact on your INR. If possible keep taking your warfarin at the correct time. If you are unwell for more than a couple of days you should get an INR check. Sometimes the INR can change very quickly if you are unwell. Remember that some anti-diarrhoea medications can interact with warfarin so check with your pharmacist or doctor before you take any additional treatment.
Diarrhoea can affect the absorption of the newer anticoagulants, so if your symptoms persist for more than 2 or 3 days you should talk to your doctor.
Have you ever mentioned any of these concerns to your doctor, or have these events occurred for you? What happened?


Leave a Reply